In this blog, we will discuss pressure ulcers, and although some may not first recognize the words “pressure ulcer”, most of us know the term “bedsore”, and that is exactly what a pressure ulcer is. Identifying risk factors and knowing what to do about them can prevent problems further down the road.
Overview of Pressure Ulcers
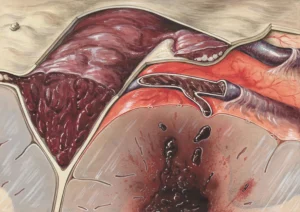 Pressure ulcers, commonly referred to as bedsores, are injuries to the skin and the underlying tissue caused by prolonged pressure on the skin. These wounds typically develop over bony areas of the body, such as the heels, hips, and tailbone. We may also hear them described as pressure ulcers or decubitus ulcers. The formation of bedsores primarily occurs when pressure limits blood flow to the skin, ultimately leading to tissue damage.
Pressure ulcers, commonly referred to as bedsores, are injuries to the skin and the underlying tissue caused by prolonged pressure on the skin. These wounds typically develop over bony areas of the body, such as the heels, hips, and tailbone. We may also hear them described as pressure ulcers or decubitus ulcers. The formation of bedsores primarily occurs when pressure limits blood flow to the skin, ultimately leading to tissue damage.
While we may typically think of these as issues primarily affecting the elderly or those who are bedridden, pressure ulcers can occur in individuals of any age who experience limited mobility or sensory impairment. The COVID-19 pandemic has significantly impacted the prevalence of pressure ulcers, as many individuals requiring long-term care or hospitalization now experience reduced mobility and increased pressure on their tissues.
Additionally, pressure ulcers have been linked to environmental factors, such as hospital settings where patients may be immobilized for extended periods. During the pandemic, healthcare systems faced unprecedented challenges, and the incidence of pressure ulcers among patients increased dramatically. This not only poses serious health risks but also places an economic burden on the healthcare system, necessitating effective strategies for management and prevention.
Recognizing where bedsores tend to develop can assist in prevention. The most common sites for these ulcers include the back and sides of the head, shoulders, elbows, hips, lower back, and areas around the knees and heels. Various demographic and health factors increase the risk of developing pressure ulcers. Individuals with limited mobility, chronic medical conditions, or those who are bedridden are especially vulnerable. Conditions such as diabetes, vascular disease, and the natural decline in skin resilience associated with aging can also contribute to an increased risk.
Key Causes and Risk Factors
The causation of pressure ulcers consist of a multitude of factors, involving a combination of external and internal forces that contribute to the injury’s formation. Externally, prolonged pressure on the skin leads to decreased blood flow, resulting in tissue damage and ulceration. Friction from the movement of skin against other surfaces and shear forces, which occur when the skin moves in a different direction than the underlying bone, are also critical factors. A common example of this is patients or elderly who are bedridden for long periods of time, hence the term “bedsores”.
Internal factors such as poor nutritional status, anemia, and chronic diseases can exacerbate the risk for developing pressure ulcers. For example, individuals with diabetes or vascular diseases may suffer from impaired blood flow, reducing the oxygen available to tissues. Age is also a significant risk factor; older adults are more susceptible due to factors like thinner skin and decreased elasticity. Other common risk factors include immobility due to neurological conditions, cognitive issues that impair a person’s ability to reposition themselves, and incontinence, which can lead to skin integrity loss.
Identifying Early Signs
Identifying the early signs of bedsores is crucial for effective intervention and management. Key symptoms to look for include changes in skin color, texture, and temperature. Initially, a bedsore might present as a localized area of skin that appears discolored. On light skin, this may manifest as a red area that does not fade when pressure is applied. In individuals with darker skin, the
discoloration may appear as purple or blue patches.
Aside from changes in color, we must observe texture changes as well. An affected area might feel warm, spongy, or hard to the touch—indications of the skin’s deterioration. We should also pay attention to temperature variation; an area that feels either cooler or warmer than surrounding skin may be an early sign of developing damage. Regularly inspecting the skin can help us identify these symptoms before they progress to more severe stages of pressure ulcers.
Understanding the Staging System
Understanding the staging system for pressure ulcers is vital, as it helps determine the severity of the wounds and informs treatment strategies. The term ‘blanch’ used below means ‘to turn white’. Generally, pressure ulcers are categorized into four stages based on depth and severity.
- Stage I: The skin is intact but may show non-blanchable redness over a localized area. The skin can feel different—warmer, cooler, softer, or firmer—than the surrounding tissue.
- Stage II: This stage involves partial thickness loss of skin, manifesting as a shallow open ulcer with a pink or red wound bed. Blisters can also be present.
- Stage III: Here, the ulcer extends into the subcutaneous fat layer. It may present as a deep crater, and the drainage may become more significant.
- Stage IV: The most severe stage, where the ulcer is full thickness and extends into muscle, tendon, or bone. The risk of systemic infection and other complications is significantly heightened at this stage.
Understanding these stages helps us determine appropriate treatment options, making it crucial for caregivers and health professionals to recognize the differences and act promptly to prevent progression.
Complications of Untreated Ulcers
The implications of untreated pressure ulcers extend beyond the immediate discomfort. Pressure ulcers can lead to serious complications, including potentially life-threatening infections. Cellulitis, a bacterial skin infection, is one such risk; if not addressed, it can progress to more severe infections like osteomyelitis, affecting the bones, or sepsis, a systemic response to infection that can result in organ failure.
Prolonged exposure to untreated pressure ulcers can result in long-term health issues that may be difficult to manage. The consequences could include persistent pain, chronic inflammation, and disability stemming from musculoskeletal complications.
Moreover, the consequences are not only physical; we must also acknowledge the psychological effects of living with pressure ulcers. The ongoing discomfort or disfigurement can lead to anxiety, depression, and a diminished quality of life for affected individuals.
Effective Prevention Strategies
Preventing pressure ulcers requires a proactive and comprehensive approach. One of the most effective strategies is repositioning regularly. Every two hours is a recommended guideline for those who are immobile; careful changes in position can relieve pressure and improve blood circulation.
In addition to repositioning, we must consider nutritional factors as critical components of ulcer prevention. Adequate hydration and a balanced diet rich in proteins, vitamins, and minerals are essential in maintaining skin integrity and overall health. Recognizing the need for balanced nutrition can be especially vital for individuals at higher risk.
Using specialized equipment, such as pressure-relieving mattresses and cushions, can also be beneficial. These products help redistribute weight and reduce direct pressure on vulnerable areas. Employing these preventive measures can significantly decrease the incidence of pressure ulcers in at-risk populations.
Treatment Approaches
When it comes to treating pressure ulcers, proper wound care is of paramount importance. General hygiene practices such as keeping the wound clean and dry are essential. This includes gentle cleaning and changing dressings regularly to foster a clean environment that promotes healing.
Medical dressings play a significant role in protecting bedsores and supporting the healing process. Various types of dressings are available, each designed to provide moisture, absorb exudate, and protect the area from infection. Creams and ointments can also be beneficial, especially those with hydrating or barrier properties.
In severe cases, surgical intervention may be necessary. Options may include debridement to remove dead tissue, reconstruction procedures to close extensive wounds, or skin grafts to repair the damaged areas. Choosing the right treatment approach depends on the bedsores’ stage and the overall health of the individual.
Preventive Measures and Best Practices
Preventing pressure ulcers is a critical aspect of patient care. We should all adopt specific routines to maintain skin integrity and prevent the formation of ulcers:
- Regular Position Changes: For individuals who are bedridden, repositioning every two hours is essential to relieve pressure. Those in wheelchairs should shift their position frequently, ideally every 15 minutes.
- Skin Care: Keeping the skin clean and moisturized is vital. Routine inspections for any signs of redness or breakdown should be undertaken to catch issues early.
- Nutrition and Hydration: A balanced diet rich in protein, vitamins, and minerals can support skin health and promote healing. Staying hydrated is equally important.
- Specialized Equipment: Utilizing pressure-relieving mattresses and cushions can help distribute weight evenly and reduce pressure points, particularly in high-risk patients.
- Education: Educating caregivers and patients about the importance of pressure ulcer prevention can help ensure everyone is vigilant with care practices.
By implementing these best practices, we can significantly reduce the incidence of pressure ulcers and enhance the quality of care for at-risk individuals.
In summary, recognizing the importance of pressure ulcer management is crucial for improving health outcomes. Through awareness of early signs, understanding staging, and implementing effective prevention and treatment strategies, we can mitigate the impact of these significant health concerns. For healthcare providers and caregivers, it is a crucial responsibility to remain vigilant and proactive in the fight against bedsores, ensuring that individuals, especially those with limited mobility, receive the care they deserve. For patients, understanding the nature and causes of bedsores can prevent future issues before they begin.
Reference
- Bedsores (pressure ulcers) – Symptoms and causes – Mayo Clinic
- Pressure ulcers (pressure sores) – NHS
- Pressure Sores: Treatment, Stages, and Symptoms – WebMD
- Bedsores (Pressure Ulcers): Symptoms, Staging & Treatment
- Pressure Sores | Bedsores | Pressure Ulcers – MedlinePlus
- Pressure Ulcer – StatPearls – NCBI Bookshelf
- Pressure Ulcers and Wounds/Injury Management
- Sepsis and Pressure Ulcers (Pressure Injuries) – Sepsis Alliance