Overview of Venous Leg Ulcers
In this blog, we will discuss venous leg ulcers- what they look like, what they are, how they form and what to do about them. Like many of the conditions we discuss in these blogs, it’s important
to discuss any questions and concerns with your doctor.
Definition and General Information
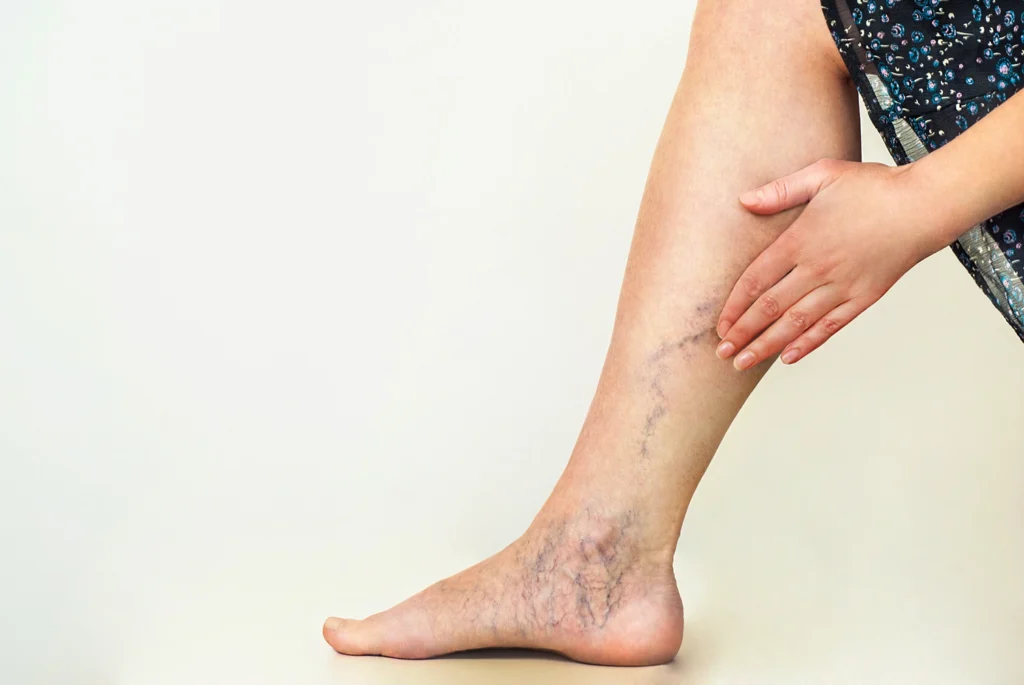 A venous leg ulcer is a type of chronic wound that typically arises due to issues related to venous blood flow. These ulcers usually occur on the lower legs, particularly around the ankle area, and are associated with chronic venous insufficiency, where the veins do not adequately return blood to the heart. Given that venous leg ulcers can take an extended period to heal—often several months or even longer—their impact on overall quality of life can be significant. Understanding their features is essential for anyone, regardless of their medical background, as early recognition can facilitate timely and effective treatment.
A venous leg ulcer is a type of chronic wound that typically arises due to issues related to venous blood flow. These ulcers usually occur on the lower legs, particularly around the ankle area, and are associated with chronic venous insufficiency, where the veins do not adequately return blood to the heart. Given that venous leg ulcers can take an extended period to heal—often several months or even longer—their impact on overall quality of life can be significant. Understanding their features is essential for anyone, regardless of their medical background, as early recognition can facilitate timely and effective treatment.
Common Locations for Development
Most venous leg ulcers develop in the lower leg, typically on the medial (inner) aspect of the ankle, although they may appear at other locations, including the calf region. The specific location of the ulcer is often indicative of underlying venous issues and can help guide treatment options.
Notably, awareness of common areas for ulcer development allows us to identify potential problems early and seek appropriate medical advice.
Importance of Early Recognition
Recognizing the signs of venous leg ulcers early is crucial. Delayed treatment can lead to further complications, including infection, increased pain, and extended healing times. Our understanding of the signs and symptoms associated with these ulcers becomes vital in preventing a simple wound from developing into a more serious health issue. Prompt medical assessment fosters better management and can significantly influence treatment outcomes.
Symptoms of Venous Leg Ulcers
Visual Characteristics of Ulcers
Venous leg ulcers often appear as irregularly shaped sores with a moist, shallow wound bed. The edges of the ulcer may be uneven, and the surrounding skin may exhibit discoloration or signs of
inflammation. The ulcer often has a reddish or brownish tint due to the presence of hemosiderin from trapped blood cells. Understanding these visual characteristics can assist us in distinguishing venous leg ulcers from other types of leg ulcers.
Common Sensations and Discomforts
Individuals with a venous leg ulcer commonly experience discomfort, which can include a dull aching sensation in the leg as well as increased pain when standing or sitting. Other sensations such as itching, burning, or a feeling of heaviness in the affected limb are also frequent. Being aware of these discomforts helps us recognize the possible onset of an ulcer and motivates us to seek medical attention without delay.
Associated Skin Changes
As we examine the skin surrounding a venous leg ulcer, we often find signs of significant change. The skin may become hardened or indurated, appear discolored, and may even develop signs of eczema or dermatitis. This crusting and color change can indicate that the ulcer is chronic and requires specialized wound care to promote healing.
Causes and Risk Factors
Underlying Venous Conditions
One of the primary causes of venous leg ulcers is chronic venous insufficiency caused by damaged vein valves that lead to poor blood circulation. This malfunction causes blood to pool in the legs, increasing venous pressure and resulting in tissue breakdown. Conditions such as deep vein thrombosis and varicose veins further exacerbate the risk of developing ulcers since they hinder proper blood flow.
Lifestyle and Genetic Factors
Certain lifestyle choices significantly influence the risk of developing venous leg ulcers. Obesity, a sedentary lifestyle with limited physical activity, and smoking can all elevate the risk. Moreover, genetic predisposition plays a role, with a family history of venous diseases likely increasing our chances of experiencing similar issues.
Age and Other Medical Conditions
As we age, our risk of developing venous leg ulcers increases. Factors such as a previous injury to the leg, paralysis, or conditions like diabetes can further elevate susceptibility. Understanding this risk landscape helps us act proactively in maintaining our leg health and seeking preventive measures, especially if we fall into higher-risk categories.
Diagnosis of Venous Leg Ulcers
Initial Assessment Procedures
Diagnosing a venous leg ulcer typically begins with a thorough physical examination by a healthcare professional. The assessment should include not just an evaluation of the wound itself, but also an inquiry into our overall health history and any conditions that may have contributed to the ulcer’s formation.
Diagnostic Tests Used
To establish a diagnosis, medical professionals may employ a range of diagnostic tests, including the ankle-brachial index (ABI) and Doppler ultrasound imaging. These tests help assess blood flow and identify potential underlying issues with the veins. By undertaking these diagnostic approaches, we receive vital information that can steer the treatment plans for venous leg ulcers.
Importance of Medical History
Our medical history plays a critical role in the diagnosis process. Information regarding previous leg injuries, existing medical conditions, and lifestyle factors can assist healthcare providers in
determining the right course of treatment. Hence, we should be prepared to provide detailed accounts of our health when seeking care for a potential ulcer.
Treatment Options Available
Standard Treatments and Medications
Treatment options for venous leg ulcers depend on severity and specific characteristics of the ulcer. Commonly, healthcare providers recommend wound care strategies, including keeping the wound clean and covered, applying topical ointments, and utilizing antimicrobial dressings if infection risk is present. Standard medications such as pain relievers may also be prescribed for discomfort management.
Advanced Therapeutic Procedures
For ulcers that do not respond to standard wound care, advanced therapeutic procedures may be necessary. Treatments such as debridement, where necrotic tissue is removed, or advanced therapies like growth factor injections can promote healing.
Additionally, referral to specialist wound care teams may help tailor treatments to our specific needs.
Role of Compression Therapy
Compression therapy is one of the cornerstones in managing venous leg ulcers. The use of compression bandages or stockings helps improve blood flow in the legs, facilitating healing while decreasing swelling. This method is essential for successful outcomes, and adhering to prescribed compression protocols significantly reduces the chance of ulcer recurrence.
Prevention Strategies
Lifestyle Modifications to Reduce Risk
Implementing lifestyle changes can vastly reduce our chances of developing venous leg ulcers. Maintaining a healthy weight, engaging in regular physical activity, and avoiding prolonged periods of inactivity can improve venous circulation.
Moreover, elevating our legs when seated or lying down can alleviate pressure on the veins, ultimately benefiting leg health.
Importance of Regular Monitoring
Regular monitoring of our leg health—especially if we have a history of venous issues—is essential in prevention efforts. Awareness of any changes in our legs or skin conditions enables us to seek prompt medical evaluations and care. Engaging with healthcare professionals regularly increases the likelihood of timely interventions should any issues arise, so be sure to contact your doctor if you notice any issues, no matter how small.
Recommendations After Healing
Even after a venous leg ulcer has healed, continued vigilance is important to prevent recurrences. Adhering to compression therapy, maintaining an active lifestyle, and following medical advice for ongoing monitoring can significantly lower the risk of the ulcer returning. We must also prioritize educating ourselves on best practices for care to promote lasting leg health- check here often for subsequent blogs and topics regarding venous leg ulcers and other relevant topics and discussions.
Living with Venous Leg Ulcers
Daily Care and Management Techniques
Living with a venous leg ulcer requires diligent self-care and commitment to daily management practices. Cleaning the ulcer, regular hand washing, and changing dressings as needed, following healthcare provider instructions, and maintaining hygienic practices contribute to successful healing. Ensuring good nutrition can also support our body’s healing processes. Practice makes perfect- and that’s also true of good health practices!
Emotional and Psychological Considerations
Beyond the physical symptoms, dealing with venous leg ulcers can take an emotional toll on individuals. Any type of long-term recovery efforts can be taxing. Feelings of frustration or anxiety about healing and potential complications are common. Support groups and counseling services can provide valuable resources for emotional support, enabling us to share experiences and coping strategies.
Support Resources and Groups
Community support is a critical component of managing venous leg ulcers. Local health organizations, wound care clinics, and online communities can offer resources, education, and connection opportunities. Engaging with these support networks not only empowers us but also enhances our understanding of effective self-management strategies.
Acknowledging the multifaceted nature of venous leg ulcers and addressing them holistically equips us with the knowledge needed for proper management and treatment. By understanding their signs, symptoms, causes, and prevention strategies, we can actively participate in maintaining our leg health and overall well-being.
Reference
1. Venous Ulcer: Symptoms, Causes, Treatment & Prevention
2. Venous Ulcers – Johns Hopkins Medicine
3. Venous Leg Ulcer – StatPearls – NCBI Bookshelf – NIH
4. Venous leg ulcer – NHS
5. Symptoms of a Venous leg ulcers – why is my leg ulcer not healing?